Best Chronic Care Management (CCM) Software Buyer's Guide 2025
Kimberly Mullen
Kimberly Mullen
The Chronic Care Management (CCM) Software integrates with and improves the efficiency of the Electronic Medical Records (EMR) software by adding features and functionalities that upkeep the Chronic Care Management service. This also enhances the existing features in the EMR systems. By incorporating CCM software system services with your EMR/PM software, you will be able to:
The purpose of the software is to save the time that you spend in manually recording and managing the chronic conditions of patients. CCM software provides better care for the patients, automated data documentation, customized treatment while making sure that your precious time never gets wasted.
The criterion mentioned below must be taken into account before qualifying a patient for CCM.
Before adopting choosing CCM software services for your practice, make sure if the software has the following main features:
Overall Coordination – A Chronic Care Management software should have team-based care and coordination among the providers.
Alerts & Consent – The software must contain initial forms and documents that aware the patients that they qualify for chronic care program and have the consent to receive treatment.
Plan Maker - An extensive plan maker for each qualifying patient with an ability to modify care plans throughout the treatment.
Risk Profile Assignment – A good Chronic Care Management Software should able to assign level. A risk level must be assigned to all patients to adjust treatment based on the level of the risk.
Claims & Billing - A CCM software must have an efficient billing process which evaluates utilized logs, patient plans, and reports and gives billing at the end of each month.
HIPAA Compliance - A top Chronic Care Management software must meet certain HIPAA regulations which ensure patient privacy. The data should be fully encrypted and the software must have antivirus protection.
CCM Dashboard - A real-time dashboard loaded with efficient features like maintaining Chronic Care Management minutes and tasks is a must for a good Chronic Care Management software.
Electronic Health Records Software or commonly referred to as EMR Software represents the electronic method of storing medical records for patients. Using specially designed software, physicians and other medical professionals can store anything ranging from patient demographics to extensive clinical information about patients, such as medical history, social history, lab reports and more.
Since all medical providers (MDs, DOs, PAs, NPs, LCSW, OT, etc.) work in a distinct manner based on their background and medical specialty, EHR Software or EMR Software must accommodate the unique style and documentation requirements. Examples of such specialty-specific features include the ability to annotate images or the capability to store before/after photos for Pain Management specialists and Dermatology specialists respectively. Similarly, other specialties such as Pediatrics, Oncology, Podiatry, Ophthalmology, Neurology, Nephrology, Dialysis Centers, Rheumatology and Chiropractic Care require their unique set of specialty-specific features to simplify adoption.
Since the introduction of the HITECH Act, healthcare IT has undergone a massive transition starting from the widely recognized Meaningful Use program to what is now known as MACRA, the Medicare EMR Incentive Program. The Meaningful Use program has transformed and now formed part of the four components of the new Merit-Based Incentive Payment System (MIPS), which itself is a fundamental part of MACRA.
For some medical practices, the transition from paper-based records to EMR Software (Electronic Medical Records Software) has not been a simple one. Regardless, realizing that the benefits of utilizing ONC Certified EHR Software far outweigh the hassle and challenges associated with it - ensuring a viable future, most practices today have successfully transformed their clinical and administrative operations to EMR Software.
Aside from ensuring tangible financial incentives and profitability, practices converting to EHR / EMR Software have seen the following benefits:
Just like a medical specialty, EMR Software requirements also depend on the size of the medical practice. From solo provider clinics to large multi-provider, multi-specialty clinics, every practice has unique inherent challenges that must be addressed by the EMR Software vendor.
A small doctor’s office not only has a limited number of staff members but their EMR Software budgets are also extremely low compared to a large enterprise such as a hospital. Due to these budgetary constraints, many providers simply choose to employ Free EMR Software or choose an affordable EHR Software vendor with a low fixed monthly fee. Cloud-based access is one such important requirement so that these providers can access patient charts even from home when needed.
These practices usually consist of 5 to 10 medical providers often belonging to the same medical specialty. Their requirements are more stringent, while their budget is also considerably large. Aside from specialty-focused requirements (EHR Software by Specialty), these practices also require unique features such as interoperability, dedicated customer support, multi-device support as well as extensive reporting functionality to keep an eye on the overall performance of the practice.
Larger group practices generally comprise more fifteen or often twenty medical providers. These practices usually provide medical services that fall under various medical specialties (Orthopedics, Pain Management, Surgery, Chiropractic Medicine, Family Medicine, etc.). Therefore, these practices require support for multiple users to access the system simultaneously, as well as for the Scheduling software to accommodate multiple locations, providers and resources such as Dialysis Chairs, procedure room allocation, etc. These practices also keep replacing or adding staff members and need a scalable solution.
EMR software companies such as Epic, Cerner, AllScripts, NextGen, Athenahealth, IMS by Meditab, eClinicalWorks, Meditech, McKesson, MEDHOST, etc. usually target and provide solutions for larger corporations like Hospitals, ACOs, PCMH, IPAs, CINs (Clinically Integrated Networks), Public Health Departments, etc.
These customers have the most elaborate list of requirements, which are usually documented in the form of an RFI or RFP to assess and shortlist vendors that can meet them. The requirements consist of features like inventory management modules, interface with local labs (LIS), machines and diagnostic equipment along with drug dispensing (pharmacy management software) and electronic medication administration records (EMAR), etc.
These entities also require the EMR software also need to integrate with multiple other software and medical devices.
Since the introduction of Meaningful Use, most healthcare practices simply have little or no choice but to convert their practice operations to EHR software. However, most providers today select the EHR software of their choice that best suits their specific needs and must perform an extensive search to evaluate all available options before they find one that is suitable. Most potential EMR Software buyers in the market today have the following in common:
Although #3 is ideal, every provider and practice workflows are unique and therefore what works for one provider may not suit the other. “One size fits all” simply doesn't apply in the world of healthcare IT. Software experts and industry specialists are an ideal source of information, advice and ultimately ensuring that the right decision is made.
EMR software includes several types of software based on specific applications or functionalities:
Small doctor offices benefit the most from cloud-based EMR software technology since minimum to no upfront cost or maintenance is required and accessing the EHR Software is possible from any location given the availability of internet access. This type of EMR software is also device dependent in most cases and can be accessed using devices such as Smartphones (Android & iOS), iPhones, iPads, laptops, and desktop computers. The move to the public cloud for healthcare is vital in the current changing landscape. For practices that do not adopt new cloud services, the old inferior feature-set coupled with the higher prices will hinder the business dramatically. This gulf between the old software and the new cloud-based software will only grow more exponentially as time goes on.
Apple dominates the digital device and computer market in the US today, so it is no surprise that many providers are specifically looking for their EMR Software vendor to support the Mac operating system (Mac EMR Software). Not all Vendors today work on a Mac device, so looking for a vendor with native support for Mac devices is essential to ensure that the software performs on existing hardware at the practice and does not require more investment in computer systems.
This is the most significant requirement for most software buyers today as the software must comply with the standards and guidelines set by the Office of the National Coordinator (ONC). Online repository details all software vendors and details related to their respective compliance with the measures set by the ONC (Click here). Software that complies with these standards have undergone rigorous testing and confirmed at a benchmark level defined by the federal body. The software testing done during this exercise checks all areas of the EMR Software system from Patient Portal access to the way the EHR Software communicates with other programs and entities like labs, Pharmacies (via e-Rx), hospitals, HIEs, etc.
With competition rising in healthcare IT, EMR software providing integrated Practice Management software as part of their overall software package easily outperforms rivals with standalone EHR Software including those that may offer a specialty-specific EHR software. EMR Software companies with integrated Practice Management solutions often provide extensive reporting capabilities to track practice performance and manage business operations better.
Medical practice has several needs of software systems to streamline operations across the board. One such important area is billing for services rendered and communications with insurance companies. Medical Billing Software, therefore, works best when integrated with the Electronic Health Records software. All clinical documentation seamlessly conforms to the required standard and forms a financial document that can be electronically sent to payers (insurance carriers) to verify and process at their end. This simplifies the operations and ensures all parties are on the same page when it comes to the financial health of the enterprise. Medical billing software helps practices and medical billing managers generate claims, patient statements, verify patient eligibility and more. This software is ideal for practices who want to handle billing in-house and can integrate with EMRs.
An EMR Software must ensure the security and safety of patient records while ensuring privacy and HIPAA compliance for patient/doctor communication (Patient Portal). This is a paramount concern for physicians and HIPAA compliance should be guaranteed at all times by the EHR Vendor. Most Vendors today (Epic, Cerner, Athenahealth, AdvancedMD, PrognoCIS, Modernizing Medicine, eClincalWorks etc.) are aware of the importance of HIPAA compliance and have taken steps to ensure the safety of patient records security in every section of the EHR Software using advanced tools like data encryption technologies to enhance the security of the EMR software.
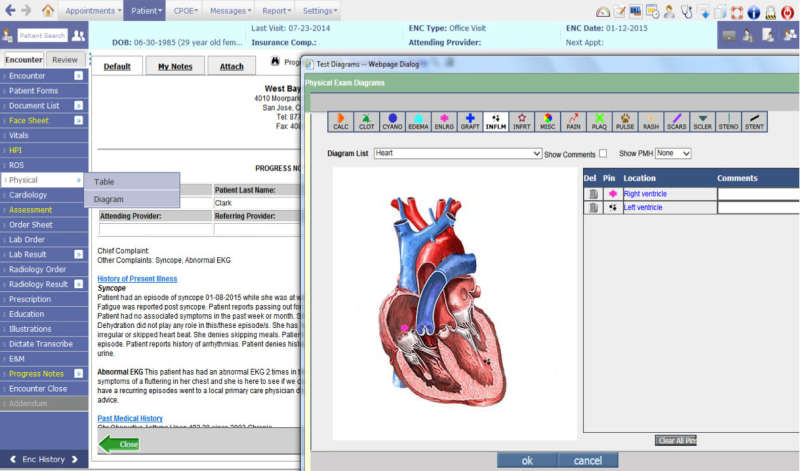
One of the decisions your practice will have to make is whether you want just EMR software or one with integrated Practice Management for billing and scheduling. There are advantages to having both together but there have been cases where some practices only go for one if they had unique requirements that a vendor could not fulfill or they had already paid a hefty amount for PM software and weren't looking to replace it yet.
Doctors are not IT professionals, and though some might be tech-savvy, it would be egregious to expect them all to be experts on the EHR software. Ease of use is essential to make the transition from paper to electronic smooth, as well as day to day practice to go along without a hitch. If the software is too complicated and hard to understand, it's a waste of precious time and needlessly aggravating. Some vendors offer free training while others don't; make sure you ask for training if your practice needs it.
Not all specialties are created equal, so why must their software be generic? Basic EHR software works well and good for general practice and most specialties, but doctors have complained about specialty specific not being available in the market. The specialty software have inbuilt recording systems that make specialty practices functioned efficiently. Only a few vendors provide specialty-specific software, so there aren't many to choose from. But the more vendors are cottoning on to the demand and there should be more options in the near future.
Support is a major issue most practices have with their current vendors. A good support team can make small glitches to major roadblocks easy to maneuver while a bad one will just make things worse. Some vendors provide support as part of the plan you are already paying for, while others charge extra for support. Scout the market, read reviews or just ask point-blank if there will be a special support team assigned to each practitioner and whether you will be charged for the service.
Smartphones have changed the dynamics of mobile usage. Handheld devices are easy to carry around and can be used for any number of uses. Most people are ditching the cumbersome PC for a handheld device. Doctors mostly use iPads or Tablets in the examination room to take down patient symptoms, check the history and note down the prescription, so it's imperative that the vendor has a mobile application that is synced with all the mobile devices being used in the practice.
There are varying price lists out there; some offer free services, while others charge an arm and a leg for specialty services. Either way, there will be hidden costs that you might get to know about later. Fix your budget and talk to vendors you interview about hidden costs within the contract and whether services such as training and support are free.
Like anything else, the EMR software industry is also subject to constant changes. From new technology to legalities and governing bodies, everything is constantly changing. Here are some of the changes I think it would do well for you to keep track of.
At a previously held health care conference Andy Slavitt, the administrator of the Centers for Medicare & Medicaid Services had declared that Meaningful Use was over, and would be replaced by the end of that year with something better. But a deeper look into the claims revealed that meaningful use was very much still there, only much improved.
The new measures aim to make the reporting and benchmark for reaching the required reports much easier and laxer than under Meaningful Use, along with other changes.
A previously conducted study had revealed how only 25% of the physicians had shown interest in the web-based EHR software systems and only 50% had adopted it as an initial model that was to ultimately transit to cloud-based software. But it has been established now, how the cloud-based EMR software cuts down the costs of having and maintaining all the hardware and client servers. It can be hosted on any device which has a web browser. That is why more and more healthcare software vendors are switching to cloud-based EHR software.
In 2025, the demand for EMR software solutions for healthcare practices has continued to rise, with market growth estimated at around 6-7% year-over-year as healthcare providers increasingly prioritize digital transformation and interoperability. This increase is largely driven by the adoption of advanced technologies like AI and cloud computing within these systems, which enhance clinical workflows and patient care. Epic Systems has expanded its dominance, now capturing over 35% of the market, particularly among large multispecialty organizations. Meanwhile, Oracle Health (formerly Cerner) has faced challenges, especially in retaining smaller hospitals, contributing to a slight decline in its market share. Together, major players like Epic, Oracle Health, Meditech and Allscripts account for a significant portion of the current EHR market.
EMR software is quickly widening their range of practice types in order to become more accessible to healthcare services. The amount of people who lack the time and knowledge, who are in health IT, is increasing each year. This makes optimizing these software solutions more difficult as they must now cater to different needs. Douglas W. Bowerman, MD, predicts we will see a “continued trend towards accessibility” in EHRs, both in terms of how we access them – on mobile, for instance – and who can access the software.
Healthcare facilities accumulate massive amounts of patient data. Patient health and financial data lets vendors help physicians with Clinical Decision Support (CDS). Leveraging analytics algorithm predictions can solve interoperability-related accessibility issues. Data warehouse development is also an opportunity to ensure more accurate patient data thanks to automation.
Despite being used more for cryptocurrency and a recent surge in NFT’s, the blockchain has recently found a place in EMR software. The blockchain allows EHR data to be secured through cryptography, making it available only to those who have access to it in the first place. As an example, the blockchain can validate clinical trial and claims results, track medicine distribution and prevent insurance fraud. Although the usage of blockchain in EHR had only just begun since the start of 2022, it is still being used to secure data and ensure confidentiality.
5G Networks are poised to become the forefront of data communication method in only a few years. They offer up to 100x the speed of contemporary 4G networks yet may still not integrate properly with the current state of healthcare. As it stands, there are many different formats available that are all competing to become the dominant method for EHR communication. As such, medical records are currently spread amongst these different formats; they are incompatible and so the various EHR systems cannot communicate at all. Until a standard is agreed upon, 5G networks will not be able to bypass the bottleneck created by two opposing systems.
The current standards that regulate EMR are very lax. Vendors end up having to pay millions in settlement fees due to false claims about meaningful use certifications. However, regulations are becoming far stricter and more transparent to prevent incidents like this happening again. The interface between physicians and medical billing coders will likely become more separate. This is because they both need access to completely unrelated pieces of information, so sharing the same regulations often leads to life - threatening miscommunication.
For EMR/EHR companies to continue to grow, it is going to require a lot more than simply using existing technology to diagnose your issues. Ensuring patients have consistent engagement throughout the scheduling process is imperative. One of the best ways to boost patient engagement is by increasing your outreach via different social mediums and making content more easily accessible, through patient communities for example. Giving physicians an insight into their patient's health has become paramount and has recently been utilized by including data from smart devices in patient reports.
Technology is innovating on a daily basis and constantly influences electronic health records. For example, common AI virtual assistants are beginning to assist healthcare services, speeding up the diagnostic process and increasing efficiency. Other tech giants are also entering the healthcare field, such as Apple and Google. With their massive budgets, they have the ability to invest heavily in R&D without taking many risks. They have also already witnessed the issues that arise from the lack of interoperability in current iterations of EMR software, and are very unlikely to make the same mistakes. This competition is great for consumers and clinicians as it will force EHR vendors to rapidly modernize their systems with far more regular updates, meaning large-scale changes are on the horizon.
Despite promising patients access to medical records, this feature has not materialized on EHR systems as of yet. A study in 2019 found that only 10% of patients who had access to their records online actually accessed them; of them, 63% were encouraged to do so by their healthcare providers. To prepare for potential regulatory changes in the future, software developers are updating EHR systems to be easier to navigate and better fit the patient's needs. Practices themselves are also now providing proper guidance and awareness about the importance of regularly checking one's own records to familiarize themselves before appointments.
EHR systems are the forefront supplier for paper-to-screen technology, so it is imperative for the software to be inclusive towards a wide range of digital capabilities. Implementing better use of data liquidity will allow data to be more accessible, increasing the EHR footprint. This can be done without sacrificing the security of the data. Implementing better interoperable solutions will also expand the footprint, allowing healthcare organizations to better access and exchange patient data.
Increasing the EHR footprint of medical practices has proven to massively improve both efficiency and savings for the industry. In 2005, a RAND study suggested that up to $77 billion could be saved by adopting EHR software. The study was so influential that previously, in 2022, more than 90% of hospitals have adopted complete use of EHR software in their practice.
In recent years, advancements in AI and machine learning have dramatically changed the healthcare industry. As these technologies continue to evolve, they are likely to have a significant impact on the future of EHR (Electronic Health Record) and EMR software. By leveraging AI and machine learning algorithms, EMR systems can become more intuitive and efficient, streamlining clinical workflows and improving patient outcomes. The application of AI and machine learning will also enable EMR systems to provide more personalized and proactive care, by analyzing patient data and identifying potential health issues early on. Additionally, these technologies have the potential to revolutionize clinical research and drug development by providing access to vast amounts of patient data and insights.
Digital Therapeutics involves software that can behaviorally alter patients and help treat mental conditions through the use of different interventions. Usually, digital therapeutics are used through smartphones and tablets. The software is quickly being integrated into EHR software and they aim to be more patient-centric. As they begin to meet industry requirements, their popularity will continue to rise and clinical trial results will continue to be published in peer-reviewed journals.
In their current state, EHR and EMR software do not properly address medical error prevention. Previously, illegible handwriting on paper prescriptions were blamed, but over-reliance on computers to supply the correct doses for medication can prove to be equally as dangerous. For example, a 16-year old patient in 2013 was prescribed 38 tablets of medication, but it turned out to be an overdose for someone of that age. These sorts of errors are far more common than we would like to believe. In the future, EMR and EHR software developers are striving to dramatically reduce these errors by de-cluttering the physician notification center which could cause less time spent attending to patients. Currently, details such as patient implants may not be added to the system before radio-logical imaging since EHRs don't actually have a standard place to store notes.
One of the biggest hassles in dealing with current EMR / EHR software is being able to easily navigate through mountains of data. Despite large leaps in technology in recent years, EMR / EHR software is clearly behind in terms of its ease-of-use and User Interfaces. Electronic Health Records are designed for easier data access than paper files, and EMR vendors are starting to implement updated iterations of their user interface in their software to better achieve this goal.
Largely spearheaded by big tech companies such as Apple, wearable devices are surging in popularity in medical fields - the market is expected to grow 26.8% from 2022 till 2028.The devices have allowed healthcare metrics to become far more accessible and have, in turn, made medical diagnosis simpler. Integrating the data from wearable devices to Electronic Health Records (EHR) has the potential to massively improve patient healthcare. The devices include various different sensors that can track body activity and monitor environmental factors. Currently, they come in many different forms, such as smartwatches, fitness trackers and specialized apps on mobile phones.
The Healthcare industry is adapting the latest technologies not to only secure, but to also provide fast and easy access for patients to their own data. Patients need to be informed and engage timely so that they will have a better trust level with their provider. To achieve greater health outcomes, we will continue to see this trend for a longer period.
Electronic Medical Records don't offer patients the ability to access their records across multiple healthcare organizations due to the lack of data-sharing standards set between different practices. This causes significant problems for patients who receive care from multiple different centers. The issue also makes diagnosis of patients harder for physicians and healthcare providers. Due to this, EMR/EHR providers are updating their software to include interoperability and integration features to allow data to be shared between these different organizations.
As we progress into 2025, cyber security in Electronic Medical Record (EMR) systems is set to become increasingly sophisticated in response to rising cyber threats. Key developments will include advanced encryption and the use of blockchain for enhanced data integrity. Artificial Intelligence (AI) will be crucial for real-time threat detection and predictive analytics, and compliance with global data protection regulations will become more critical, necessitating adaptive strategies from EHR providers. Additionally, user training will gain prominence to mitigate risks associated with human error. Overall, the focus will shift towards building a proactive, resilient digital healthcare environment, fortified against emerging cyber challenges.
The trend in EMR (Electronic Medical Record) software is gravitating towards increased customization and modular design. This shift is driven by the diverse and evolving needs of healthcare providers across various specialties. Customizable EMR systems will allow medical professionals to tailor interfaces and functionalities to their specific workflows, enhancing efficiency and reducing cognitive load. Modular EMR systems will offer flexibility, enabling healthcare facilities to integrate only the modules they need, such as telemedicine, billing, or patient engagement tools, thereby avoiding the complexities of one-size-fits-all solutions. This approach not only improves user satisfaction but also facilitates better patient care by providing clinicians with tools that are more aligned with their practice needs. Ultimately, this evolution will lead to more adaptable, efficient, and user-friendly EMR systems in the healthcare industry.
EMR systems' ability to lower healthcare costs and increase efficiency is becoming increasingly clear as we move deeper into the digital healthcare era. Clinical workflows are predicted to be greatly streamlined by EMR systems by 2025 and beyond saving a substantial amount of time and money on administrative duties. Its effectiveness allows medical professionals to concentrate more on patient care rather than paperwork, which also results in cost savings for healthcare facilities. Effective treatment plans and preventive care strategies can be developed at a lower cost by utilizing the advanced analytics capabilities of EMR systems. To further reduce costs, it is projected that the integration of EMR systems with other digital health tools will reduce the number of redundant tests and procedures. EHR systems, in short, have the potential to play a major role in advancing the development of a healthcare system that is both more effective and affordable.
Getting closer to the digital healthcare era, the use of EMR systems in public health is becoming more and more crucial. EMR systems are essential for improving disease surveillance and management since they give real-time access to patient data in a variety of healthcare settings. EMRs are predicted to be essential tools for monitoring public health trends in the future, allowing medical professionals to quickly recognize and address new health emergencies like epidemics or patterns of non-communicable diseases. They make it easier to gather and analyze vast amounts of health data, which is necessary for developing policies and making well-informed decisions on public health. EMRs also help with the effective distribution of resources and the evaluation of public health interventions' efficacy. EMR systems are crucial in forming a proactive and data-driven approach to public health because they function as a bridge between individual patient care and population health management.
The adoption and localization of EMR systems are becoming key factors in transforming healthcare delivery. In 2025 and on-wards, a significant trend will be the customization of EMR systems to meet the specific needs of different regions and countries. This includes adapting to various languages, cultural norms, and legal requirements, ensuring that EMR systems are not only universally accessible but also relevant to local healthcare contexts. In developing regions, EMRs are expected to leapfrog traditional healthcare infrastructure challenges, offering an efficient way to manage patient data and improve healthcare delivery. The localization will also involve integrating region-specific medical practices and protocols into EMR systems, enhancing their utility and acceptance among healthcare providers. This global adoption, coupled with thoughtful localization, is crucial for creating a more interconnected and efficient global healthcare system, where patient data can be seamlessly exchanged across borders, leading to improved health outcomes worldwide.
The integration of EMR systems with emerging technologies is poised to revolutionize the healthcare sector. Advanced technologies like Artificial Intelligence (AI), machine learning, and blockchain are increasingly being incorporated into EMR systems to enhance their capabilities. AI and machine learning algorithms are being used for predictive analytics, improving diagnostic accuracy, and personalizing patient care plans. Blockchain technology is emerging as a key player in securing EMR data, ensuring tamper-proof records and enhancing patient privacy. Additionally, the integration of Internet of Medical Things (IoMT) devices is facilitating real-time health monitoring and data collection, directly feeding into EMR systems for more comprehensive patient profiles. These technological integrations not only promise to streamline healthcare operations but also aim to significantly improve patient outcomes by providing more accurate, efficient, and secure healthcare services.
The synergy between mobile health and Electronic Medical Record (EMR) accessibility is set to redefine healthcare delivery. The proliferation of smartphones and mobile devices has paved the way for mobile health apps that seamlessly integrate with EMR systems, enabling patients to access their health records, schedule appointments, and communicate with healthcare providers from anywhere. This mobile accessibility is crucial for enhancing patient engagement and empowerment, promoting transparency in healthcare services. For healthcare providers, mobile Electronic Health Records (EHR) access facilitates the delivery of care outside traditional settings, supports decision-making with real-time data, and enhances coordination among care teams. This integration is also vital in remote and under-served areas, where mobile solutions can bridge gaps in healthcare access. Moving forward, the continued evolution of mobile health coupled with EMR accessibility will play a pivotal role in making healthcare more patient-centered, efficient, and accessible globally.
As the healthcare industry continues to evolve into 2025 and beyond, the focus on sustainability and Green IT in the context of Electronic Medical Record (EMR) systems is gaining unprecedented momentum. The integration of sustainable practices and green technologies within EMR infrastructures is not only aimed at reducing the environmental footprint of healthcare IT operations but also at enhancing system efficiency and reducing operational costs. Energy-efficient data centers, cloud-based services, and virtualization are becoming key components in making EMR systems more eco-friendly. These technologies help minimize the energy consumption and carbon emissions associated with the storage and processing of vast amounts of medical data. Additionally, the push towards digital records over paper significantly reduces waste and resource use. As the industry moves forward, the adoption of Green IT practices in EMR systems will be crucial in achieving a sustainable, cost-effective, and environmentally responsible healthcare sector.
The ethical considerations surrounding the use of Electronic Health Record (EHR) systems are becoming increasingly critical. The confidentiality and privacy of patient information stand at the forefront of these concerns, demanding stringent security measures to protect sensitive data from unauthorized access and breaches. In addition to privacy, there is a growing emphasis on equity and fairness in EMR accessibility, ensuring that all patients, regardless of socio-economic status or geographical location, benefit equally from the technological advancements in healthcare. Furthermore, the integrity of patient information raises ethical questions about the accuracy and completeness of records, highlighting the importance of maintaining high standards in data entry and management. Ethical use of EHR also encompasses the responsible application of predictive analytics and AI, ensuring that these technologies do not introduce bias or compromise patient care. As the healthcare sector continues to embrace digital transformation, navigating these ethical challenges with a patient-centered approach will be paramount in fostering trust and delivering equitable, high-quality care.
The integration of precision medicine and genomics into healthcare practices is becoming increasingly vital. Precision medicine's aim to tailor treatment and prevention strategies to individual genetic profiles is revolutionizing patient care. This personalized approach is heavily reliant on the integration of genomic data into Electronic Health Record (EHR) systems, allowing for seamless access to patient genetic information by healthcare providers. Such integration facilitates the identification of genetic predispositions to diseases, enabling earlier and more targeted interventions. Furthermore, it supports the development of customized treatment plans that are more effective and have fewer side effects. The ethical management of this sensitive genetic data, ensuring privacy and informed consent, remains a paramount concern. As we move forward, the fusion of precision medicine and genomics with digital health records promises to enhance the effectiveness of healthcare delivery, making it more personalized, predictive, and preventive.
Navigating deeper into the digital era, enhancing data security and privacy within healthcare systems, particularly in Electronic Medical Record (EMR) platforms, has emerged as a paramount concern. The surge in digital health data necessitates robust security measures to protect sensitive patient information from cyber threats and breaches. Innovations in encryption technologies and the adoption of blockchain are pivotal in fortifying EMR systems against unauthorized access, ensuring that patient records are both secure and tamper-proof. Furthermore, stringent adherence to data protection regulations, such as HIPAA in the United States, reinforces the legal framework for privacy and security. Educating healthcare professionals on best practices for data handling and implementing advanced user authentication mechanisms are critical steps in mitigating risks. As healthcare continues to embrace technology, prioritizing data security and privacy will be essential in maintaining patient trust and upholding the integrity of healthcare delivery.
The concept of cross-sector data integration is becoming increasingly essential for achieving holistic health outcomes. Integrating data from diverse sectors such as healthcare, social services, and environmental agencies into Electronic Health Record (EHR) systems enables a more comprehensive understanding of the factors influencing individual and community health. This holistic approach facilitates the identification of social determinants of health, such as socioeconomic status, education, and living conditions, which are crucial for tailoring preventive and therapeutic interventions. The challenge lies in developing interoperable systems that can seamlessly exchange data while maintaining strict privacy and security standards. As we move forward, leveraging big data analytics and AI will be key in synthesizing these vast datasets to provide actionable insights. Embracing this cross-sectoral data integration will not only enhance patient care but also foster a proactive, preventive healthcare model that addresses all facets of health determinants.
The role of EMR (Electronic Medical Record) systems in disaster response is becoming increasingly crucial. In the face of natural disasters, pandemics, and other emergencies, the ability of EMR systems to provide quick and reliable access to patient records can significantly enhance the efficiency and effectiveness of healthcare delivery. By ensuring continuity of care, EMR systems help healthcare providers quickly retrieve patient histories, allergies, medications, and other critical information, even when traditional infrastructure is compromised. Additionally, cloud-based EMR systems offer resilience and accessibility, enabling healthcare professionals to coordinate care across different locations seamlessly. Integrating EMR systems with emergency response protocols and mobile health units can further bolster their utility in crises. As the frequency and severity of disasters increase, the advancement and integration of EMR systems in disaster preparedness and response will be vital in safeguarding public health and ensuring timely, coordinated medical interventions.
Natural Language Processing (NLP) is playing an increasingly vital role in enhancing Electronic Medical Records (EMR) systems by improving how healthcare providers interact with digital records. By enabling computers to understand and interpret human language, NLP facilitates more efficient documentation processes, allowing clinicians to dictate notes and automatically convert them into structured data. This technology reduces the administrative burden on healthcare professionals and minimizes the risk of errors associated with manual data entry. NLP also allows EMR systems to extract valuable insights from unstructured data, such as clinical notes and patient narratives, helping providers identify trends and make more informed decisions. Moreover, NLP algorithms can assist in coding and billing processes by accurately interpreting medical terms and procedures, ensuring compliance with regulatory standards.
EMR software designed for chronic care management (CCM) has incorporated features to support the continuous care of patients with chronic conditions. Care plan management tools allow providers to create and monitor personalized care plans, setting goals and tracking progress. Integration with remote patient monitoring devices enables the collection of real-time health data, such as blood glucose levels and blood pressure, facilitating timely interventions. Collaborative platforms within the EMR promote interdisciplinary communication among healthcare teams, ensuring coordinated care. Patient portals provide educational resources and self-management tools, empowering patients to take an active role in their health. Analytics capabilities assist in identifying population health trends and evaluating the effectiveness of CCM programs.
Chronic Care Management EMRs are utilizing AI to provide proactive patient care. Predictive analytics identify patients at risk of disease exacerbation, enabling timely interventions. AI-driven virtual assistants engage patients in self-management, offering personalized health tips and medication reminders. These features enhance patient engagement and contribute to better chronic disease management.